MarketsMarketWatchApr 21, 2026· 2 min read
Medicare's $50 GLP-1 Program Faces Insurer Pushback Over Economic Burden
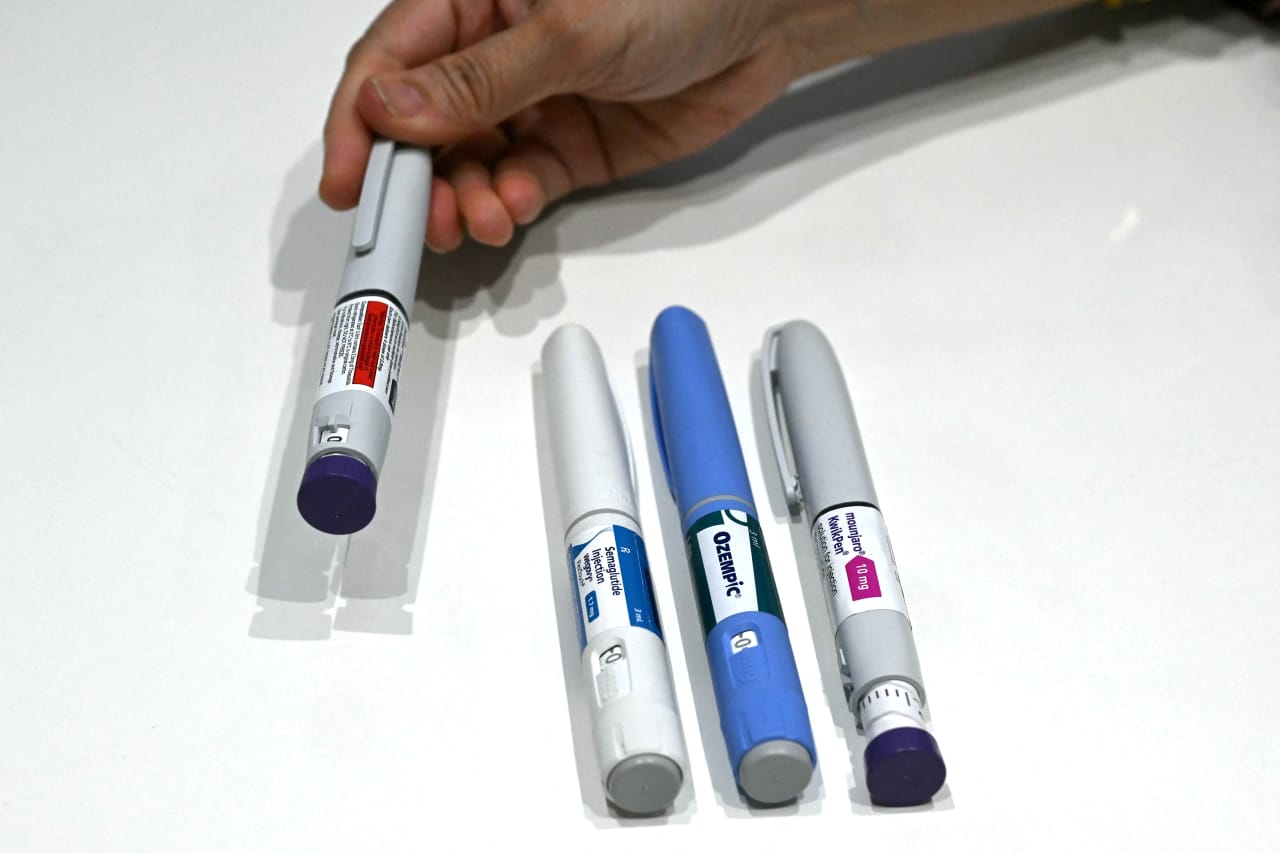
Medicare's new program allowing seniors to access GLP-1 medications for weight loss at $50 per month is drawing concerns from health insurers regarding financial sustainability. Insurers are questioning the immediate cost burden and its impact on Part D plans, weighing it against potential long-term healthcare savings from improved beneficiary health.
Medicare's forthcoming program, designed to offer beneficiaries GLP-1 medications for weight loss at a subsidized rate of $50 per month, is encountering significant resistance from a segment of health insurers. This initiative, intended to broaden access for seniors, is sparking a robust economic debate within the healthcare industry concerning its financial sustainability and wider market impacts.
Currently, most Medicare Part D plans do not cover GLP-1s specifically for weight management, thus limiting accessibility for many eligible seniors. While the new program substantially enhances affordability for beneficiaries, insurers are raising pertinent questions about the potential for substantial cost increases. These plans, which administer a significant portion of Medicare benefits, anticipate a notable surge in demand for these high-cost medications once the $50 co-payment threshold is widely implemented.
The economic implications of this policy are multifaceted. For beneficiaries, the program represents a considerable reduction in out-of-pocket expenses for drugs that typically exceed $1,000 monthly, potentially leading to improved health outcomes and an enhanced quality of life. From a public health economics perspective, expanded access to GLP-1s could theoretically lead to a reduced incidence of obesity-related comorbidities such as Type 2 diabetes and cardiovascular disease, potentially lowering overall long-term healthcare expenditures across the system.
However, insurers are primarily focused on the immediate financial burden. They contend that absorbing the majority of these drug costs could significantly strain their balance sheets and potentially necessitate higher premiums or a reduction in benefits elsewhere within Part D plans. The central economic discussion revolves around whether the projected long-term health cost savings from improved weight management will adequately offset the immediate, substantial increase in pharmaceutical expenditures, and how these costs will ultimately be distributed across the Medicare system and its private partners. The rollout of this program is poised to notably reshape the economic landscape of pharmaceutical coverage for seniors and the operational strategies of Medicare-affiliated health plans.


